To understand this, we first need to define Bioequivalence is the absence of a significant difference in the rate and extent to which the active ingredient becomes available at the site of drug action when the same dose is given under similar conditions. Essentially, if two drugs are bioequivalent, they do the same thing in your bloodstream at the same speed.
What Exactly is the 80-125% Rule?
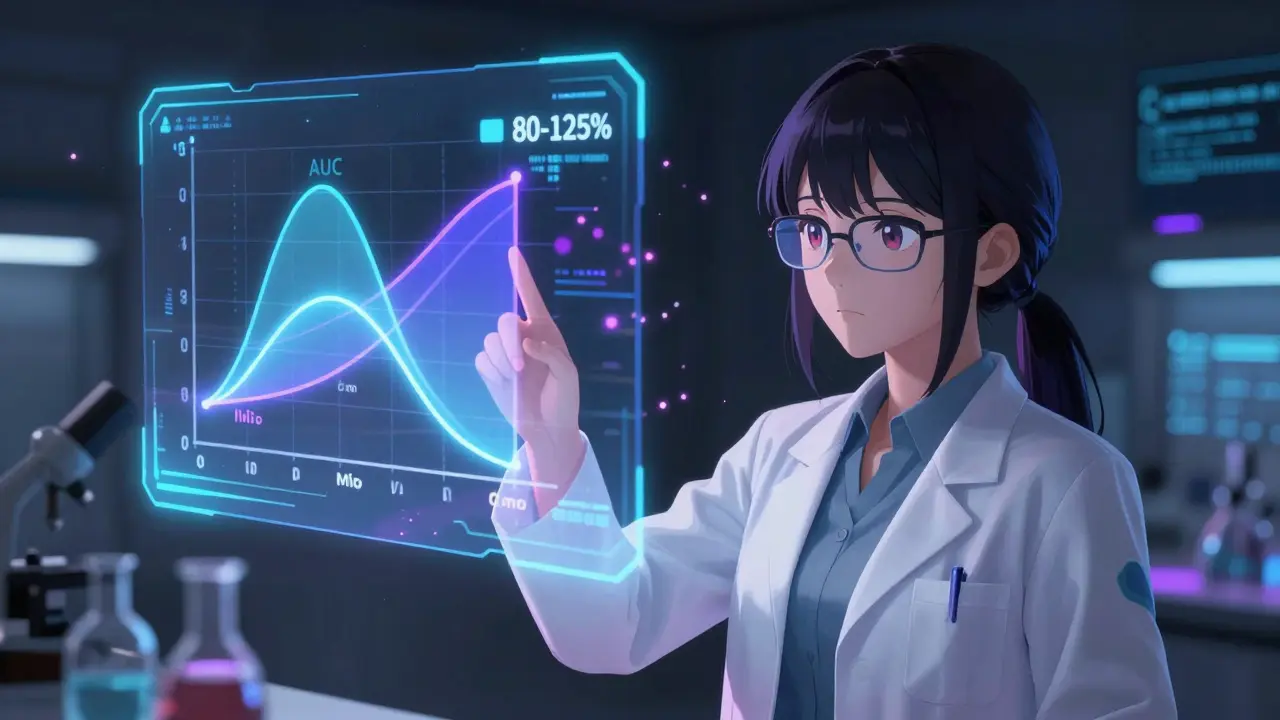
The 80-125% rule is the global gold standard used by the FDA (U.S. Food and Drug Administration) and the EMA (European Medicines Agency) to ensure generics work as well as the brand name. It requires that the 90% confidence interval (CI) of the ratio of the geometric means for two key markers-AUC and Cmax-falls entirely between 80% and 125%.
Wait, why 90%? Most people are used to the 95% confidence interval seen in general science. However, the bioequivalence confidence intervals use 90% because it allows for a 5% statistical error at both the top and bottom limits. This creates a total error margin of 10%, which regulators have found to be the sweet spot for ensuring safety without making the testing process impossible.
Here are the two primary markers that must either hit this range:
- AUC (Area Under the Curve): This measures the total amount of drug that reaches the bloodstream. If the AUC is within 80-125%, the total exposure is considered equivalent.
- Cmax (Maximum Concentration): This measures the peak level of the drug in the blood. It tells us how fast the drug is absorbed.
The Math Behind the Magic: Why Log-Transformation?
If you look at raw pharmacokinetic data, it's often messy. Drug absorption doesn't follow a neat, bell-shaped curve (a normal distribution); instead, it follows a log-normal distribution. This means if scientists just averaged the numbers, the results would be skewed.
To fix this, researchers use a process called logarithmic transformation. Once the data is "logged," the 80-125% range becomes symmetric around zero on a log scale (specifically from -0.2231 to 0.2231). This mathematical trick allows statisticians to apply standard tests to data that would otherwise be too erratic to analyze accurately.
| Metric | What it Measures | Regulatory Goal | Impact of Failure |
|---|---|---|---|
| AUC | Total Drug Exposure | 80-125% CI | Ineffective dose or toxicity |
| Cmax | Absorption Rate (Peak) | 80-125% CI | Too slow to work or acute side effects |
Is This "One Size Fits All" Approach Fair?
For most drugs, the 80-125% rule is incredibly robust. A 2022 meta-analysis of 214 studies confirmed that products meeting this standard showed no clinically meaningful differences across 37 drug classes. But not every drug is the same. Some are "narrow therapeutic index" (NTI) drugs, meaning a tiny change in blood levels can be the difference between a cure and a crisis.
For NTI drugs like Warfarin (a blood thinner) or Levothyroxine (thyroid hormone), the 80-125% range is often too wide. In these cases, the FDA may require a tighter window, such as 90-111%, to ensure patient safety. Similarly, "highly variable drugs"-those that fluctuate wildly even in the same person-might use a Scaled Average Bioequivalence (SABE) approach, which can expand the limits based on the drug's natural variability.
Clearing Up the Biggest Misconception
Let's address the elephant in the room: the belief that a generic pill can contain 20% less active ingredient than the brand name. This is simply not true. In a 2022 survey, over 60% of community pharmacists actually held this mistaken belief.
There is a massive difference between content uniformity and bioavailability. Content uniformity is the actual amount of powder in the tablet; generics usually must contain 95-105% of the label claim. Bioequivalence, however, is about what happens *after* you swallow the pill. The 80-125% rule applies to the pharmacokinetic behavior in the body, not the recipe in the factory. You aren't getting 80% of a drug; you're getting a drug that is absorbed with 80-125% of the efficiency of the original.

How Bioequivalence Studies Actually Work
Getting a drug approved isn't just about a few tests. A typical study involves a randomized, crossover design with 24 to 36 healthy volunteers. These volunteers take the brand drug, wait for a "washout period" so the drug leaves their system, and then take the generic version (or vice versa).
This process is time-consuming and expensive. It usually takes 8-12 weeks to conduct the study and another 4-6 weeks for statistical analysis. For pharmaceutical companies, this adds millions of dollars and up to two years to the development timeline. But this rigor is why generic drugs now account for about 90% of prescriptions filled in the U.S. while remaining safe and effective.
Does the 80-125% rule mean my generic drug is less potent?
No. The rule does not refer to the amount of active ingredient in the pill. Most generics contain nearly the same amount of active medication as the brand name (typically 95-105%). The rule describes the range of how the drug is absorbed and processed by the body, ensuring that the clinical effect is the same.
What happens if a drug's confidence interval is 79-126%?
If the 90% confidence interval falls even slightly outside the 80-125% range, the drug is generally not considered bioequivalent. In such cases, the FDA or EMA would likely deny market access unless the company can prove the difference is clinically irrelevant or adjust the formulation to fit the criteria.
Why is a 90% confidence interval used instead of 95%?
The 90% CI is used to balance statistical rigor with practical reality. It allows for a 5% error at each end of the spectrum. This standard was chosen by regulatory experts because a 95% CI would be overly restrictive, potentially blocking generic drugs that are therapeutically identical but fail a stricter mathematical test.
Are all generic drugs subject to the same 80-125% rule?
Most are, but there are exceptions. Narrow Therapeutic Index (NTI) drugs often require tighter limits (like 90-111%) because small changes in blood concentration can be dangerous. Highly variable drugs may use "scaled" limits, and some simple immediate-release tablets can get a waiver if they pass strict dissolution tests in a lab.
What are AUC and Cmax in simple terms?
AUC (Area Under the Curve) is like the total volume of water that flowed through a pipe over an hour-it's the total exposure your body gets to the drug. Cmax is like the highest pressure the pipe ever reached-it's the peak concentration of the drug in your blood at its strongest moment.
Next Steps for Researchers and Patients
If you're a clinical researcher, the biggest pitfall to avoid is skipping the log-transformation of your pharmacokinetic data. Without it, your results will be statistically invalid. Also, remember that both AUC and Cmax must meet the criteria simultaneously; if only one passes, the study fails.
For patients, the takeaway is simple: trust the process. While a 20% window sounds large, it's a statistical boundary for a 90% probability, not a random guess at the dosage. If you are taking an NTI drug and feel a difference when switching generics, talk to your doctor, as you may be one of the few people who require a tighter tolerance than the standard rule provides.


Melinda Hawthorne
I work in the pharmaceutical industry as a research analyst and specialize in medications and supplements. In my spare time, I love writing articles focusing on healthcare advancements and the impact of diseases on daily life. My goal is to make complex medical information understandable and accessible to everyone. Through my work, I hope to contribute to a healthier society by empowering readers with knowledge.
view all postsWrite a comment